Can Your Pelvic Floor Be Too Tight? What You Need to Know
You’ve been told your tests are normal. You don’t have an infection. Your scans are clear. And yet something is wrong — sex is painful, your bladder won’t cooperate, or you’re struggling with constipation that no one can explain. The answer might lie somewhere most doctors don’t think to look: your pelvic floor muscles.
For a significant number of women, the problem isn’t a weak pelvic floor. It’s one that is too tight — chronically tense, unable to relax, and responsible for a surprisingly wide range of symptoms that are frequently missed or misdiagnosed.
Written by Sangita Patel, Sports and Women’s Health Associate Physiotherapist at Vitality Physiotherapy — with over 20 years’ clinical experience in physiotherapy including pelvic floor rehabilitation
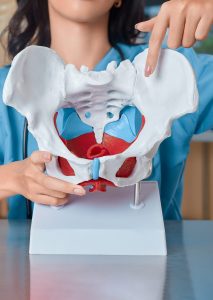 How can tight pelvic floor muscles cause so many different symptoms?
How can tight pelvic floor muscles cause so many different symptoms?
The pelvic floor is a group of muscles, ligaments and connective tissues that form the base of the pelvis. Like any muscle group in the body, these muscles need to be able to both contract and fully relax. When they’re held in a state of persistent tension — unable to properly let go — they can affect everything in the surrounding area: your bladder, bowel, hips, lower back, and sexual function.
This is called pelvic floor overactivity. And crucially, tight pelvic floor muscles are not the same as strong ones. Many women with this condition have muscles that are both tight and weak — shortened from chronic tension, but lacking the functional strength needed for everyday activity.
Think of a bicep that’s permanently flexed. It isn’t strong in any useful sense — it’s just stuck. A muscle that can’t fully release can’t generate real power, and the pelvic floor is no different.
Why does this happen?
Tight pelvic floor muscles rarely have a single cause. Common contributing factors include:
- Chronic stress and anxiety — the pelvic floor braces in response to stress, just as other muscles do
- Pain guarding — after injury, surgery, difficult childbirth, or chronic pelvic pain, the body protects the area through sustained tension
- History of trauma — including sexual trauma, which can create persistent protective tension patterns
- Too many Kegel exercises — excessive or incorrectly performed Kegels can worsen tightness in women who are already overactive
What are the symptoms of tight pelvic floor muscles?
This is where things get complicated — and where so many women are let down by the system. The symptoms of a tight pelvic floor overlap significantly with other conditions, which is why they’re so frequently missed.
Pain during sex
Pain during or after sex — known clinically as dyspareunia — is one of the most common presentations of tight pelvic floor muscles. Some women experience difficulty with penetration entirely, a condition called vaginismus. If sex is painful and you’ve been told there’s no physical reason for it, your pelvic floor muscle tension is worth investigating.
Pelvic pain
Persistent aching, pressure, or sharp pain in the pelvis, vagina, rectum or tailbone — especially pain that worsens with sitting — can be associated with tight pelvic floor muscles. The tailbone connection is particularly well established: several pelvic floor muscles attach directly to the coccyx, meaning muscle tension can directly contribute to coccyx pain. Clinically, some women also present with hip, lower back or groin pain that hasn’t resolved through standard treatment
Bladder symptoms that feel like a UTI — but aren’t one
This is one of the most underrecognised presentations. Tight pelvic floor muscles can mimic a urinary tract infection almost exactly, producing urgency, frequency, and even a burning sensation — without any infection being present. If you’ve repeatedly been tested for a UTI and the results keep coming back clear, tight pelvic floor muscles may be responsible.
Other bladder symptoms include:
- Always needing to pee but very little coming out
- An urgent need to pee that’s difficult to control
- Needing the toilet more than 8 times a day
- Difficulty starting to urinate, or a weak stream
- Bladder pain with no infection found
- Urgency leakage — rushing to the toilet and not quite making it
Bowel symptoms
Tight pelvic floor muscles directly affect bowel function. If the muscles can’t relax properly when you need them to, the result can be:
- Constipation with no obvious dietary cause
- Straining to open your bowels
- A feeling of incomplete emptying after a bowel movement
- Changes in stool shape or consistency
- Painful bowel movements
Pelvic pain after running or exercise
If you experience pelvic pain, or discomfort during or after exercise, tight pelvic floor muscles may be contributing
Painful periods
Dysmenorrhoea — painful periods — can also be worsened by pelvic floor muscle tension, particularly if there is underlying pelvic pain between cycles.
⚠️ A word on urgency leakage
Many women with tight pelvic floor muscles experience urgency incontinence — the sudden desperate need to urinate, sometimes with leakage before reaching the toilet. This is frequently treated with standard strengthening exercises, which can make symptoms significantly worse. If urgency is part of your symptom picture, specialist assessment is essential before starting any pelvic floor exercise programme.
How is it diagnosed?
Tight pelvic floor muscles are diagnosed through clinical assessment by a trained women’s health physiotherapist. There is no blood test or scan that will identify it. A standard GP examination will not typically detect it. This is a significant reason why many women live with these symptoms for months or years without receiving the correct diagnosis.
What an assessment involves
A specialist pelvic floor assessment will include:
- A detailed history — symptoms, onset, aggravating and easing factors, bladder and bowel habits, sexual function, stress and lifestyle
- External assessment — posture, breathing patterns, abdominal tension and pelvic alignment
- Internal examination (with consent) — direct assessment of muscle tone, tenderness, and crucially, the ability to relax
- Functional testing — how the pelvic floor responds to load, movement and breath
The internal examination is the most informative part of the assessment. It allows your physiotherapist to feel directly whether the muscles are holding excess tension and whether you can achieve a full, voluntary release. While internal examination is the most ideal, if you do not feel comfortable, we can assess in other ways.
What to expect
An internal pelvic floor assessment is carried out with your full informed consent and can be stopped at any time. It is not the same as a gynaecological examination. Your physiotherapist will explain every step before proceeding, and you are always in control. Many women are surprised by how straightforward and informative it is — and how much clarity it brings after months of unexplained symptoms.
Kegels making things worse? Here’s why
If you’ve been doing pelvic floor exercises and your symptoms have not improved — or have got worse — a tight pelvic floor is very likely the reason. This is not uncommon, and it is not your fault.
Kegel exercises are designed for pelvic floor weakness. For women whose muscles are already too tight, doing more Kegels is like asking a tensed bicep to work harder. It doesn’t improve function — it deepens the problem and frequently worsens symptoms.
This is why the generic advice to “just do your Kegels” can be actively harmful for a significant proportion of women. Without a proper assessment, it’s impossible to know whether someone needs more contraction or more relaxation. Both types of dysfunction are common. Both require a different approach.
If you’ve been doing Kegels and things have got worse, please stop and seek a specialist assessment before continuing.
How are tight pelvic floor muscles treated?
The good news is that tight pelvic floor muscles respond very well to specialist physiotherapy. For most women, symptoms can be significantly reduced — or resolved entirely — with the right approach.
The focus is on relaxation, not contraction
Treatment is fundamentally different from standard pelvic floor rehabilitation. The goal is to restore the muscle’s ability to fully release, reduce areas of tenderness and trigger point activity, and re-establish the normal contraction-relaxation cycle.
 Treatment typically includes:
Treatment typically includes:
- Relaxation techniques — guided methods to teach the pelvic floor to let go, often the most unfamiliar skill for women who have been chronically bracing
- Breathing retraining — the diaphragm and pelvic floor work together; restoring healthy breathing mechanics is foundational to reducing pelvic floor tension
- Nervous system regulation — because tight pelvic floor muscles are often strongly linked to the stress response, addressing this component is frequently essential for lasting change
- Gradual strength work — once the muscle can relax properly, functional strength can be carefully reintroduced where needed
- Soft tissue release and trigger point therapy — hands-on internal and external work to directly reduce muscle tension
How long does treatment take?
This varies depending on the severity and duration of symptoms and how consistently the home programme is followed. Many women notice meaningful improvement within 6–12 weeks. More complex or long-standing presentations may take longer. Your physiotherapist will give you a realistic individual prognosis at your initial assessment.
✅ What treatment at Vitality Physiotherapy looks like
We begin with a thorough assessment to confirm whether tight pelvic floor muscles are driving your symptoms, and to identify contributing factors. From there, we build a structured treatment plan combining in-clinic treatment with a carefully guided home programme. We work at a pace that’s appropriate for you — you fully informed at every stage.
Q6 When should I seek help?
If you recognise yourself in any of the symptoms described above, a specialist pelvic floor physiotherapy assessment is the right next step. You do not need a GP referral to be seen privately, and you do not need a confirmed diagnosis before booking.
Seek specialist assessment if you have:
- Bladder symptoms — urgency, frequency, incomplete emptying, or recurrent UTI-like symptoms with no infection found
- Constipation, straining, or incomplete bowel emptying alongside pelvic symptoms
- Pain during or after sex, or difficulty with penetration
- Pelvic, hip, tailbone or low back pain that hasn’t been explained or resolved
- Pelvic pain during or after running or exercise
- Symptoms that have worsened since starting pelvic floor exercises
- Been told everything is normal — but you know something isn’t right
Tight pelvic floor muscles are a genuine clinical condition that deserves proper assessment and individualised treatment. It is not something to push through, manage alone, or assume will resolve on its own.
Think this might be you? Specialist pelvic floor assessment — London SE1 Book a pelvic floor physiotherapy assessment at Vitality Physiotherapy vitality-physio.co.uk
Sangita Patel is a Chartered Physiotherapist (MCSP, HCPC) and Sports and Women’s Health Physiotherapist at Vitality Physiotherapy. With over 20 years’ specialist experience across sports and women’s health physiotherapy, including pelvic floor rehabilitation, she has assessed and treated hundreds of women with pelvic floor conditions.
The information in this article is for educational purposes and does not constitute individual medical advice. If you are experiencing symptoms, please seek assessment from a qualified women’s health physiotherapist.

