Why Your Back Isn’t as Fragile as You’ve Been Told
By Janine Enoch, Founder and Clinical Director, Vitality Physiotherapy
You’ve had a scan. The report mentions disc degeneration, a bulge, or some other finding that sounds alarming. Your GP or a previous clinician may have warned you to be careful, to avoid certain movements, to protect your back. And now you’re frightened — not just of the pain, but of making things worse.
Here’s what we want you to know: your back is almost certainly far stronger and more resilient than you’ve been led to believe. The evidence on this is now very clear, and it changes everything about how we approach low back pain at Vitality Physiotherapy.
What the spine actually looks like
The lumbar spine — the lower back — is made up of five vertebrae connected by facet joints that allow you to flex, extend, bend sideways, and rotate. Between each vertebra sits an intervertebral disc, long cast as the villain in the back pain story.
You’ve probably heard the phrase ‘slipped disc.’ It’s one we don’t use, because it isn’t accurate. Discs don’t slip. They are anchored firmly in place by strong ligamentous attachments. A better way to picture a disc is as a car tyre: thick, fibrous outer walls surrounding a more gel-like centre. Robust. Designed to absorb load and enable movement.
Discs can bulge or sustain injury — but this is far less catastrophic than the language around it implies.
What scans actually show us
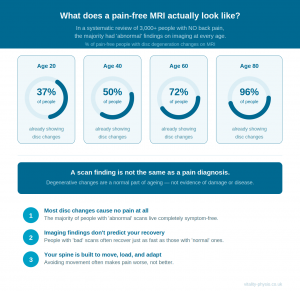
This is where the science gets genuinely surprising. A landmark systematic review examined imaging findings in over 3,000 people who had no back pain whatsoever. Here’s what they found:
- By age 40, around 50% of pain-free people had disc degeneration visible on MRI
- By age 50, the majority showed disc bulges — without any symptoms
- Facet joint changes and other ‘degenerative’ findings were similarly common across all age groups
The conclusion is unavoidable: degenerative changes on imaging are a normal part of ageing, not a diagnosis. A finding on a scan does not tell you why you are in pain, or even whether it is responsible for your pain at all.
Treating a scan result rather than a person is one of the most common mistakes in back pain management — and one we are very careful to avoid.
The posture myth

Few beliefs about back pain are more entrenched — or less well supported — than the idea that posture causes pain. For decades, patients have been told to sit up straight, to avoid slouching, to buy ergonomic chairs, and to never cross their legs.
The research does not back this up. A study of over 1,100 teenagers found no association between sitting posture and pain. In adults, even workers required to maintain awkward positions for sustained periods show no reliable increase in back pain risk. Experts cannot even agree on what constitutes ‘bad’ posture — the concept owes more to military tradition than to biomechanical evidence.
There is no perfect posture. There is no perfect chair. What matters is that you move — regularly, in a variety of ways, and without fear.
So why does back pain happen?
Back pain is real and it can be genuinely debilitating. But the cause is rarely structural fragility. In the next articles in this series, we explore the neuroscience of pain, the crucial relationship between load and capacity, and what the evidence says about treatment and exercise.
The starting point, though, is this: your spine is not broken. It was built to move, to load, and to adapt. And that is exactly what we help you do.
If you have been told your back is damaged and you’re not sure what to do next, our team at Vitality Physiotherapy can offer a thorough assessment and a clear, evidence-based plan. Clinics in Southwark (SE1) and Esher (KT10).

