Why There’s No Single Best Exercise for Back Pain — And What That Means for You
By Janine Enoch, Founder and Clinical Director, Vitality Physiotherapy
If you search online for the best exercises for back pain, you’ll find confident, contradictory advice in abundance. Pilates. Yoga. McKenzie method. Core stability. Dead bugs. Deadlifts. Walking. Swimming. Everyone has a favourite, and most of them claim the evidence is on their side.
Here’s the honest truth from the research: no single exercise type has been shown to be consistently superior for low back pain in the long term. And understanding why that is actually liberates you to focus on what really matters.
What the Studies Show
Pilates vs. Stationary Cycling
A well-designed study compared Pilates to stationary cycling over eight weeks. Both groups improved in pain, disability, and catastrophic thinking. At eight weeks, the Pilates group showed better results. At six months, the difference had disappeared.
This pattern — early advantage for the more ‘specific’ or ‘targeted’ intervention, no long-term difference — appears repeatedly in the back pain literature. It may reflect the power of receiving treatment that feels relevant and purposeful, rather than any specific physiological superiority.
Walking vs. Back-Strengthening Exercises
In another study comparing a simple walking programme to specific back-strengthening exercises, both groups improved similarly. For previously sedentary people, general movement may be as valuable as targeted exercise — because getting moving at all is the intervention.
High Load vs. Low Load
A randomised controlled trial comparing high-load and low-load motor control programmes found better short-term outcomes in the low-load group, but no meaningful difference at 12 or 24 months. Both groups also received pain education, which may have been the most influential component.
What a Systematic Review Found
A comprehensive review of the exercise literature concluded that whole-body programmes — combining strength, resistance, and general movement — had beneficial effects for back pain. Not because of any single mechanism, but because exercise in general is more effective than most passive alternatives.
Why Core Stability Exercises Aren’t the Whole Answer
Core stability has dominated back pain rehabilitation for years, and it isn’t without value. But the evidence has complicated the picture. Studies show that improvements from core exercises are often unrelated to actual changes in abdominal muscle function. The benefit may come from factors like increased confidence, exposure to movement, and the therapeutic relationship — not from ‘switching on’ a specific muscle.
More concerning, an excessive focus on core bracing and spinal stiffness may inadvertently reinforce the very protective guarding that perpetuates pain. People with back pain already tend to show increased muscle co-activation and reduced spinal movement. Training them to brace harder is not always the right answer.
Reduced movement variability — moving in a more rigid, restricted way — is consistently associated with persistent back pain. The goal, for many patients, is actually to feel safer moving freely: to decrease stiffness, not increase it.
So What Should You Do?
The best exercise for back pain is the one you will do consistently, that you find manageable and — ideally — enjoyable. Beyond that:
- Variety matters: combining different movement types, loads, and intensities tends to produce better long-term outcomes than any single modality
- Pain education matters: in almost every high-quality study, groups receiving pain education alongside exercise did better than those doing exercise alone
- Consistency matters more than perfection: a good programme done regularly beats a perfect programme done sporadically
- Your whole life matters: sleep, stress, nutrition, and relationships all influence how your body responds to exercise and how quickly you recover
The Vitality Physiotherapy Approach
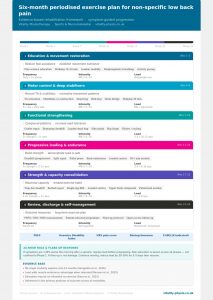 We don’t have a house exercise for back pain. What we have is a framework: assess the whole person, understand their presentation (how irritable is the pain? what are their goals? what does their daily life look like?), and design a programme that introduces load progressively, builds capacity over time, and adapts as they improve.
We don’t have a house exercise for back pain. What we have is a framework: assess the whole person, understand their presentation (how irritable is the pain? what are their goals? what does their daily life look like?), and design a programme that introduces load progressively, builds capacity over time, and adapts as they improve.
We use a macro and microcycling approach to treatment planning — structuring rehabilitation in phases, with clear goals at each stage, and building in the flexibility to adjust based on how an individual is responding. No two programmes look the same. This programme (alongside)is for informational purposes only and does not constitute medical advice. If you are experiencing back pain, please consult a qualified physiotherapist.
Jas’s Story
Ten years ago, I met Jas — a woman in her late 50s who had just been diagnosed with osteoporosis. Her bone density scans showed a T-score below -2.5, and her fracture risk was classified as high. She was frightened. She loved being active, and the diagnosis felt like a threat to everything she wanted her life to look like.
We started carefully. Weight-bearing and resistance exercises, introduced gradually, progressing as her capacity grew. Regular reassessment. Small adjustments. Alongside her rehabilitation, she made changes to her diet — increasing calcium-rich foods and vitamin D — to support what her body was working hard to do.
There were hard days. But her consistency never wavered.
When Jas returned for her annual review, her scans told a different story. She had moved from osteoporosis into the osteopenia range — a clinically meaningful improvement and a real reduction in fracture risk. Her bones had responded exactly as the evidence predicted: progressively, with appropriate load, given sufficient time.
Jas’s story is one of the highlights of my career. Not because what we did was complicated — it wasn’t. But because it worked precisely because we respected the body’s need for gradual adaptation, built a programme around her as a person, and trusted the process.
That is what good rehabilitation looks like. And it is available to everyone.
Ready to find out what a personalised, evidence-based back rehabilitation programme looks like for you? Get in touch with the team at Vitality Physiotherapy. Clinics in Southwark (SE1) and Esher (KT10).

