Long Covid: Fatigue- helpful information and how Physio can help

The Therapies for Long COVID (TLC) Study Group (the University of Birmingham), recently summarised the current research on the symptoms, complications, and treatment of long COVID.
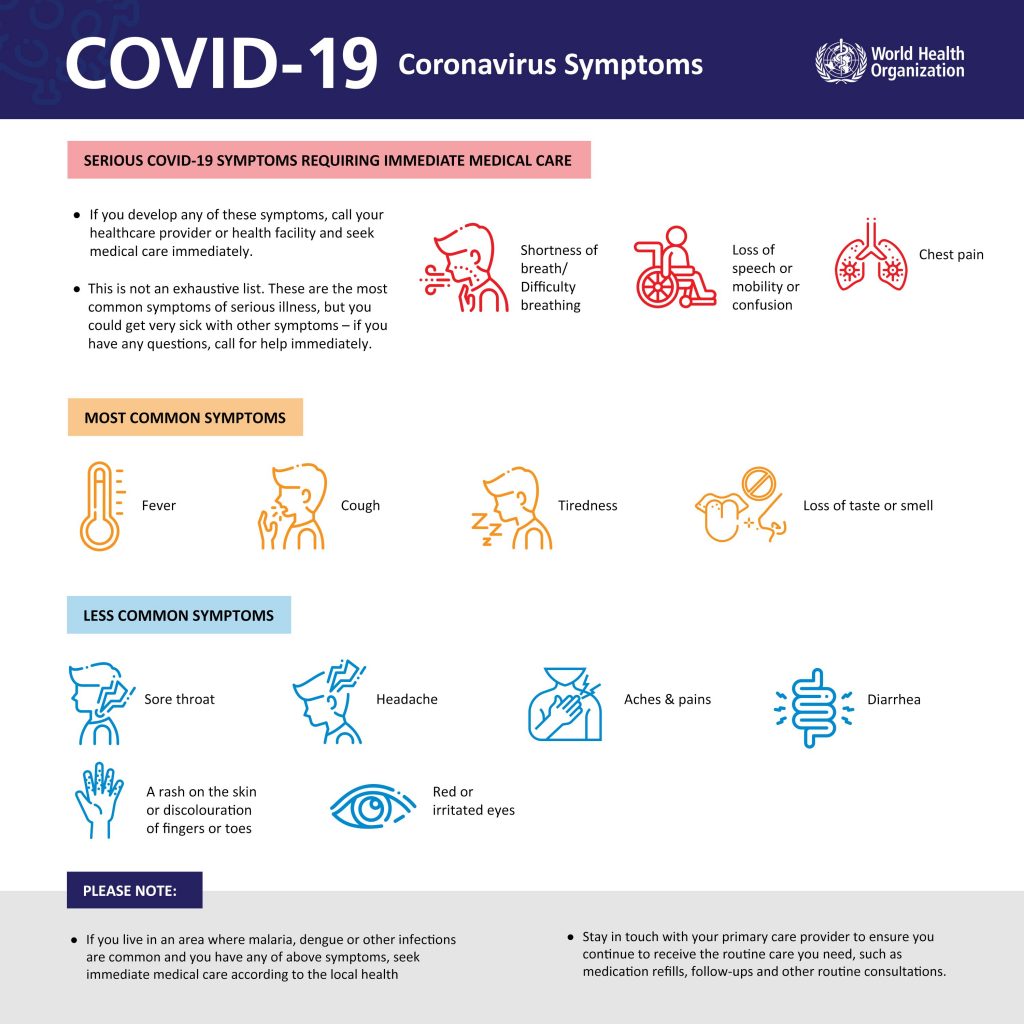
The ten most common symptoms of Long COVID were highlighted as fatigue, shortness of breath, muscle pain, cough, headache, joint pain, chest pain, altered smell, diarrhoea, and altered taste.
The two main symptom clusters for people experiencing Long COVID were:
- fatigue, headache, and upper respiratory complaints.
- ongoing fever and gastroenterological symptoms.
What is fatigue?
Fatigue is a feeling of constant tiredness or weakness, that does not improve with rest. Despite the fact that fatigue is sometimes referred to as tiredness, fatigue is not the same as being tired or sleepy.
A person often will feel fatigued for a number of reasons, whether it is physical, mental, or a combination of both. People of all ages will experience fatigue at some point in their lives.
In the case of viral infections such as COVID-19, fatigue is a normal part of the body’s response. After an infection is cleared, fatigue sometimes persists for some time. Fatigue can make you sleep more, feel unsteady on your feet, it can make exercise very difficult and affect your ability to concentrate and remember.
What causes post-viral or Long covid fatigue?
We now think that (based on post-mortem SARS research), the virus crosses the blood brain barrier.
 Proposed Mechanism of how Long Covid causes fatigue by Vitality Physiotherapy
Proposed Mechanism of how Long Covid causes fatigue by Vitality Physiotherapy
The blood-brain barrier is a specialised boundary between the blood supplying the brain and the spaces between the cells of the brain (the extracellular matrix). This incredibly specialised feature of the brain is very sensitive and selective. It allows very few substances to move from the blood into the brain, stopping toxins and harmful substances from entering the brain. It allows useful substances such as water, glucose, and oxygen to enter the brain. For more detailed information on this important mechanism, watch this:
https://www.youtube.com/watch?v=e9sN9gOEdG4
The current idea about how the virus probably enters the brain is that when the virus enters your nose, it travels through the olfactory (nasal pathway). Then, it travels through the soft tissue in the nose via the drainage mechanism of the brain (lymphatic system). It may also possibly explain why anosmia (lack of ability to smell) is observed in patients with COVID-19.
Pro-inflammatory substances, such as cytokines (interferon gamma, and interleukin 7) start to increase in the brain area. This seems to affect the glymphatic system (macroscopic waste clearance system that use tunnels around blood vessels, formed by astroglial cells (star-shaped nerve cells), to help rid the brain of soluble proteins, waste, and metabolites from the central nervous system. The glymphatic system (largely active whilst we sleep) also helps deliver glucose, lipids (fats), proteins, growth factors, and neuromodulators to the brain. This is one of the reasons why we as humans need quality sleep because many of the toxins in our brains are eliminated when we do so.
The cytokines likely pass through the blood-brain barrier in organs such as the hypothalamus, leading in the longer term to interruption of the sleep/wake cycle, cognitive dysfunction and profound fatigue (post-exertional malaise), all characteristic of Chronic Fatigue Syndrome Myalgic Encephalomyelitis (CFS/ME).
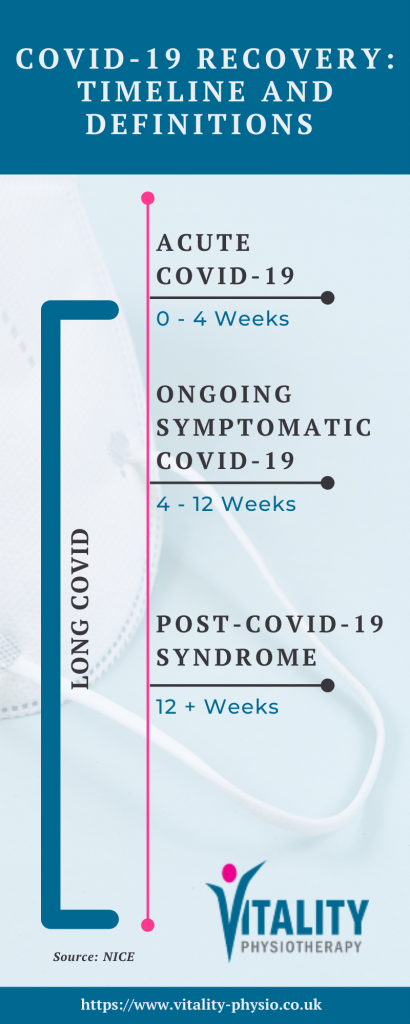
We think that as it was the case with the SARS outbreak, some patients who contracted the COVID-19 virus may go on to develop a severe post-viral syndrome we term ‘Post COVID-19 Syndrome’ or Long COVID
What can I do to help myself?
There are many interventions and self-management strategies to help with ongoing fatigue after recovering from your initial infection.
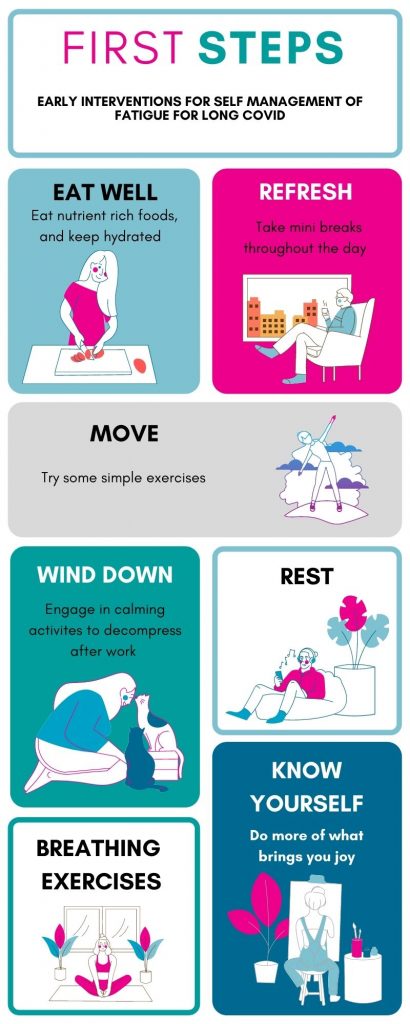
Nutrition
Eat regular healthy nutrient-rich foods including fresh vegetables, fruit, carbohydrates, and healthy fats. Vitamin D has been shown to decrease viral load and boost your immune system, so get some sun too! Remember that your body is comprised of between 50 and 65% water and it is crucial to your recovery to keep topped up.
Refresh
A short break every few hours is so beneficial to enhance your wellbeing and productivity. A mini-break does not need to be complicated. It can simply be a few minutes away from your work; this may be chatting with someone who is in the room with you or getting a drink, looking at a piece of art, listening to music, doodling, or drawing.
Sleep
Sleep is critical to your recovery because when you sleep your immune system works more efficiently. Our sleep hygiene top tips are to ensure you train your body to get to sleep every night at the same time, keep your room as dark as possible, avoid caffeine after 2 pm and stop using screens at least an hour before bed.
Move
Get active, initially, it might just be a gentle 5 min stroll or a few simple arm exercises, but you can slowly build up your activity levels. A little exercise often, allowing periods of rest in between activities is a great way to start. If you’re back at work, try standing up from your desk, if you’re office-based, every hour and march on the spot. Try going for a walk every day, starting with 5 min or so, and gradually increasing your walk time
If however, you find that simple exercises like climbing up a single flight of stairs, leaves you breathless, speak to your GP. If you feel like after exercise, you experience exceptional fatigue and malaise, speak to one of our Physios, about a more structured exercise plan, that may involve goal setting, exercise tolerance prescription, and pacing.
Wind down, allow time
The severity of the virus is not directly proportional to the level of fatigue you may be experiencing. We are all ‘wired’ differently, and our experience of illness is not the same. There is no carbon copy reference, so don’t rush with your rehab. Some patients experience levels of anxiety, fear, or even sadness. Decompress your thoughts by engaging in calming activities such as meditation, prayer, relaxing with a pet, or listening to music. Activating your creative brain too, or by being “inflow” has been shown to help many people with their levels of happiness. Drawing, writing, and other repetitive creative activities activate “flow” and produce dopamine, which is a feel-good chemical that energises and motivates you.
Breathing exercises
Many of us over breathe, taking more oxygen than we require and in turn, can experience chronic fatigue. Mouth breathing is one of the biggest culprits that cause us to over breathe. Nasal breathing, on the other hand, is a more effective, more efficient method of breathing. Its benefits are vast in number and include improved lung volumes, reduced exposure to foreign substances, improve the function of your diaphragm, improve athletic performance, sleep better, and have better-smelling breath!
Check out this video about nasal breathing by our in-house respiratory Physiotherapist, Janine Enoch:
Finally,
If you are experiencing fatigue with exercise, diminished tolerance for exercise, or simply confused about where to start, speak to one of our Physiotherapists for a free 15 min chat, which we can do over the phone or in person. Help is at hand, live well with Vitality Physiotherapy.