Why Do I Leak When I Run? A Physiotherapist Explains
Written by: Tamara Figaji Women’s Health Physiotherapist with over 20 years experience working with female athletes
| If you leak urine when you run, jump or exercise, you are not alone — and it is not something you simply have to accept. This is called stress urinary incontinence, and it is one of the most common — and most treatable — conditions seen in women’s health physiotherapy. This article explains exactly why it happens and what you can do about it. |

First: You Are Not Alone
Many women — including fit, active, athletic women — experience urinary leakage during running or high-impact exercise. Research suggests that up to 1 in 3 women who exercise regularly experience some form of stress urinary incontinence, and among female runners the figure is even higher.
It is also one of the most under-reported problems in women’s health. Many women quietly stop running, avoid certain classes, or start wearing pads without ever seeking treatment — often assuming it is just a normal part of having had children, or getting older.
It is common. It is not normal. And in the vast majority of cases, it is highly treatable.
What Is Actually Happening When You Leak
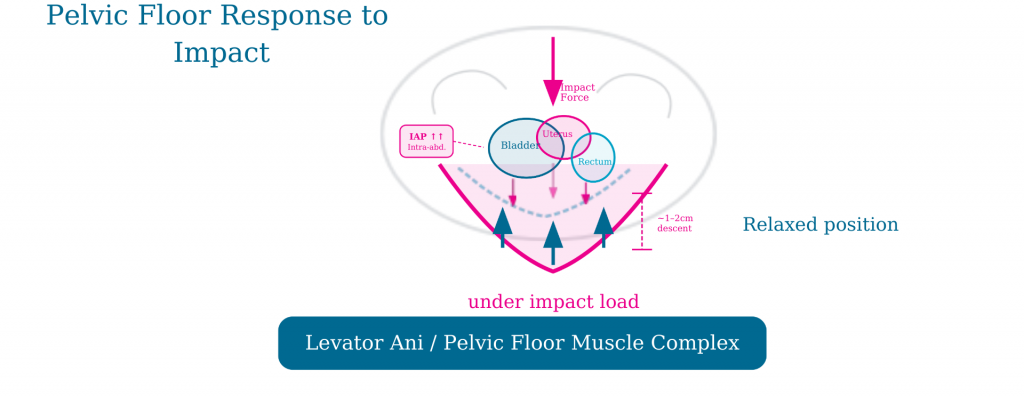
Every time your foot hits the ground during a run, a significant force travels up through your body. Running generates ground reaction forces of two to three times your body weight with each stride. At the same time, your diaphragm descends and intra-abdominal pressure spikes rapidly.
Your pelvic floor — the group of muscles that sit at the base of your pelvis — is responsible for managing that pressure and maintaining closure of the urethra. In a well-functioning pelvic floor, these muscles contract reflexively just before and during impact to counterbalance the pressure and keep you dry.
When leaking occurs during running, it means that reflex is not working well enough. This can be due to one or more of the following:
- The pelvic floor muscles lack sufficient strength to generate the required closing force
- The muscles are poorly coordinated — they contract too late, or not at all during impact
- The muscles are actually overactive or tight, which paradoxically reduces their ability to generate force
- The load demand of running exceeds the current capacity of the pelvic floor
- Hormonal changes (especially around menopause or postnatally) have affected tissue quality
| Important: Leaking during running is not always caused by weakness. Some women leak because their pelvic floor is too tense — a distinction that matters enormously for treatment. This is why a proper assessment is essential before starting any exercise programme. |
Why Running Specifically?
Running is a high-impact, repetitive activity that creates more pelvic floor loading than most other forms of exercise. Studies have measured the impact forces involved and found running to be significantly more demanding on the pelvic floor than cycling, swimming, or even the elliptical trainer.
This is why many women can manage a gym session, a yoga class or a walk without any leakage — but find running triggers symptoms. It does not mean running is damaging. It means your pelvic floor’s capacity has not yet caught up with the demand being placed on it.

Other factors that can make symptoms worse during running:
- Running on hard surfaces (more impact than trail running)
- Running pace — faster running increases impact forces
- Fatigue — pelvic floor endurance decreases as you get tired
- Hydration and bladder volume — a fuller bladder is harder to manage
- Recent childbirth or hormonal changes that have altered tissue support
Is It Just About Having Had Children?
Childbirth — particularly vaginal delivery — can stretch, strain or partially disrupt the pelvic floor muscles and their nerve supply. This is a significant factor for many women who leak when running. However, it is not the only cause.
Women who have never been pregnant can also experience stress urinary incontinence, particularly elite and recreational female athletes. The cumulative load of high-impact training over time, combined with other hormonal and structural factors, can be sufficient on its own.
Menopause is another major contributor. The decline in oestrogen affects the elasticity and thickness of pelvic and urethral tissues, making the pelvic floor less responsive and more vulnerable to leaking under load.
What Can Be Done About It
The good news is that stress urinary incontinence during running responds very well to physiotherapy. NICE guidelines — the clinical standards that govern healthcare in the UK — recommend pelvic floor muscle training as the first-line treatment for stress urinary incontinence before any other intervention is considered.
When delivered by a specialist women’s health physiotherapist, pelvic floor rehabilitation has been shown to significantly reduce or eliminate leakage in the majority of women — including those who have been dealing with the problem for years.
What treatment actually involves:
- A thorough assessment of your pelvic floor function — not just strength, but coordination, timing and relaxation ability
- A personalised rehabilitation programme tailored to your specific deficit
- Functional training that bridges the gap between pelvic floor exercises and running — because Kegels alone rarely solve a running-specific problem
- Load management: how to continue running while your pelvic floor capacity builds
- Breathing and pressure management strategies to reduce the spike in intra-abdominal pressure during impact
- Strength work targeting the glutes, hips and deep core — which all support pelvic floor function
Most women see meaningful improvement within 6 to 12 weeks of structured, progressive rehabilitation. Some see results much sooner. The key word is structured — the evidence consistently shows that supervised physiotherapy produces significantly better outcomes than self-directed exercise.
Are Kegels Not Enough?
This is one of the most common questions — and the honest answer is: often not, when the goal is returning to running.
Kegel exercises — or pelvic floor contractions — are a starting point. But they train the pelvic floor in isolation, in a static position, with no load. Running places high-speed, high-load demands on the pelvic floor in a dynamic, upright position. The gap between those two things is significant.
Effective rehabilitation for running-related leakage needs to include progressive loading — squats, single-leg work, impact preparation, and eventually a graded return to running programme. It also needs to address timing and coordination, not just strength.
Many women also either over-squeeze (creating a muscle that is tight but not strong) or perform the contraction incorrectly without knowing. An assessment with a specialist physiotherapist ensures you are working in the right direction from the start.
When to Seek Help
You should seek a pelvic floor assessment if:
- You leak any amount of urine when running, jumping or exercising
- You have had to modify or stop running because of leaking
- You are wearing pads during exercise
- You are postnatally and preparing to return to running
- You are perimenopausal or postmenopausal and noticing new or worsening symptoms
- You are not sure whether what you are doing as self-treatment is helping
Early intervention makes a significant difference. The longer symptoms persist without treatment, the more compensatory habits can develop — adjusting your running gait, reducing speed, avoiding certain routes — which can create secondary issues over time.
Frequently Asked Questions
Can I keep running while being treated?
In most cases, yes. Your physiotherapist will advise on load management — which may involve temporarily modifying distance, pace or surface — while your pelvic floor capacity builds. Complete rest from running is rarely necessary or recommended.
How long will treatment take?
Most women see meaningful improvement within 6 to 12 weeks of structured rehabilitation. Some see changes sooner. The timeline depends on the severity of symptoms, how long they have been present, and consistency with the home programme.
Do I need an internal examination?
Not necessarily — but it can provide very valuable information about muscle tone, coordination and strength that cannot be assessed externally. It is always optional, consent-based, and explained clearly beforehand. Many women find it far less daunting than expected.
Is leaking during running a sign of prolapse?
Not always — they are separate conditions, though they can co-exist. Stress urinary incontinence and pelvic organ prolapse are both related to pelvic floor function but have different presentations. An assessment will clarify what is contributing to your symptoms.
I had a C-section — can I still have pelvic floor problems?
Yes. While vaginal delivery carries more direct risk to the pelvic floor, pregnancy itself places significant load on the pelvic floor regardless of how you delivered. C-section also involves abdominal surgery that can affect deep core function and scar tissue mobility.
I have been leaking for years — is it too late to treat?
No. Long-standing stress urinary incontinence can still respond well to pelvic floor rehabilitation. The duration of symptoms does not determine whether treatment will work — though it may affect how long it takes to see full resolution.
| Ready to run without leaking? Book a Women’s Health Assessment at Vitality Physiotherapy in Southwark or Esher. A 60-minute specialist appointment to assess your pelvic floor, understand your symptoms, and create a personalised plan to get you back to running confidently. |
